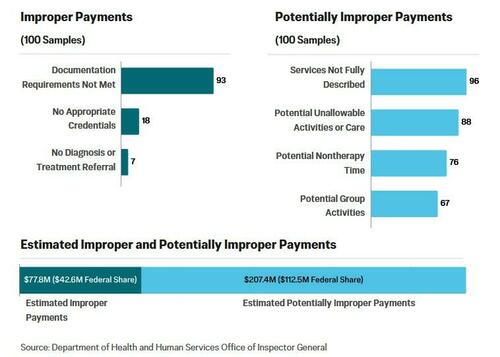
A recent federal audit has brought to light a deeply troubling landscape within Colorado’s Medicaid program, revealing an estimated $77.8 million in improper payments and an additional $207.4 million in potentially improper payments for autism therapy services. The February report, issued by the Inspector General for the Department of Health and Human Services (HHS OIG), paints a stark picture of systemic failures in oversight and program integrity, raising serious questions about the stewardship of taxpayer funds and, critically, the safety and quality of care provided to vulnerable children with autism spectrum disorder and developmental disabilities.
The audit, which scrutinized $289.5 million in Medicaid payments made between 2022 and 2023 for over one million claims related to Applied Behavior Analysis (ABA) therapy, found a staggering 100 percent failure rate among the sample claims reviewed. Every single one of the 100 claims examined contained at least one improper or potentially improper payment, underscoring a pervasive lack of adherence to federal and state requirements. This unprecedented rate of non-compliance indicates a profound breakdown in the administrative and clinical processes intended to ensure that Medicaid funds are used judiciously and that beneficiaries receive appropriate, medically necessary care.
Unpacking the Financial Irregularities and Claim Errors
The distinction between "improper" and "potentially improper" payments is crucial for understanding the audit’s findings. Improper payments are defined as those claims that definitively failed to meet established federal or state requirements, irrespective of intent. This could include payments for services not rendered, services not medically necessary, or payments that did not comply with billing rules. Potentially improper payments, on the other hand, refer to claims so poorly documented or unreliable that auditors could not verify whether the services were correctly provided or even occurred. The sheer volume of both categories points to widespread issues, ranging from administrative sloppiness to potential fraud, waste, and abuse within the program.
A detailed breakdown of the audited claims revealed a litany of errors, each contributing to the substantial financial discrepancies and highlighting critical vulnerabilities in the system:

- Pervasive Documentation Failures: In an overwhelming 93 out of 100 claims, billing providers either neglected to furnish proper notes verifying that therapy sessions actually took place, failed to secure required signatures from therapists or supervisors, or billed for more time than their own internal notes indicated. Adequate documentation is the cornerstone of any healthcare billing system, ensuring accountability, transparency, and proof of service delivery. Its absence makes it impossible to verify the legitimacy of claims.
- Provision of Care by Unqualified Personnel: A significant concern arose in 18 cases where therapy services, specifically those requiring the expertise of a specialist such as a Board Certified Behavior Analyst (BCBA), were instead delivered by staff lacking the necessary qualifications and credentials. ABA therapy is a highly specialized intervention, and the qualifications of providers are paramount to ensuring its effectiveness and ethical delivery.
- Absence of Medical Necessity Documentation: In seven instances, children receiving therapy lacked a current doctor’s diagnosis or referral on file. A physician’s diagnosis and referral are fundamental prerequisites for establishing medical necessity, which dictates whether a service is eligible for Medicaid reimbursement. Without these, the appropriateness of the therapy itself comes into question.
- Billing for Non-Medical and Recreational Activities: A particularly egregious finding involved 88 cases where facilities billed Medicaid for activities explicitly not considered medical therapy. These included academic tutoring, general daycare services, or custodial care. In one striking example, a facility sought reimbursement for children participating in swimming and playing on water slides. Medicaid is designed to cover medically necessary services, and its funds are not intended for recreational or educational activities that fall outside this scope. This practice diverts resources from legitimate medical care.
- Inaccurate Timekeeping and Billing Practices: In 76 cases, facilities billed for a full eight-hour day of therapy without properly deducting time for essential breaks, meals, or naps. This "full-day billing" without accounting for natural human needs inflates service hours and leads to overpayments, demonstrating a fundamental disregard for accurate time management and billing protocols.
Systemic Oversight Failures and Their Consequences
The OIG report emphatically concludes that Colorado’s Medicaid program made these improper payments primarily due to a profound lack of effective oversight. Several key areas of deficiency were identified:
- Insufficient Regular Payment Reviews: The state did not implement regular, robust reviews of Medicaid payments for autism therapy to proactively identify and rectify errors. Without consistent auditing mechanisms, discrepancies can proliferate undetected, allowing improper practices to become entrenched.
- Unclear Guidance to Therapy Centers: A significant contributing factor was the state’s failure to provide clear, unambiguous guidance to therapy centers regarding appropriate billing practices and what constitutes reimbursable therapy under Medicaid. Ambiguity in regulations can lead to confusion, unintentional errors, or, in some cases, deliberate exploitation.
- Inadequate Monitoring of Prior Authorization Contractors: The state also failed to properly monitor its prior authorization contractors, who are responsible for approving therapy for children before services are rendered. Prior authorization is a critical gatekeeping mechanism designed to ensure medical necessity and prevent unnecessary or inappropriate services. A breakdown in this oversight layer allows potentially flawed or unneeded treatments to be approved, leading to further waste.
This constellation of oversight failures created an environment ripe for error and potential abuse, ultimately undermining the integrity of the state’s Medicaid program for autism therapy.
Grave Safety and Quality of Care Concerns
Beyond the financial impropriety, the audit unearthed deeply alarming issues that directly impact the safety and quality of care provided to some of Colorado’s most vulnerable residents: children with autism. The report highlighted instances where staff members, directly involved in providing care, possessed criminal convictions that should have immediately disqualified them from working with children in a healthcare setting.
- Criminal Histories Among Care Staff: The audit revealed that some staff members had criminal convictions for serious offenses, including weapons offenses, assault, and driving under the influence (DUI). In one particularly disturbing case, three staff members at a single facility providing care to an 11-year-old child with autism had documented criminal histories.
- Felony Convictions and Direct Child Contact: One non-credentialed technician was found to have a felony weapons offense conviction just three months prior to treating children. Another registered behavior technician had a conviction for misdemeanor assault and physical harassment. A third behavior technician had an aggravated misdemeanor weapons conviction. These individuals, with histories of violence or serious criminal behavior, were entrusted with the care of children who often have communication challenges and may be particularly vulnerable to abuse or neglect.
- Absence of Background Checks: The root cause of this alarming situation was identified as the state’s failure to require comprehensive background checks for these workers. This systemic gap meant that individuals with dangerous criminal records could gain access to children in therapeutic settings without any protective screening mechanism in place. The absence of such a fundamental safeguard represents a critical breach of duty and places children at unacceptable risk.
The implications of these safety concerns extend far beyond financial waste, striking at the very core of trust and protection that healthcare programs are expected to provide. For parents of children with autism, who often rely heavily on these services, the revelation that their children might be cared for by individuals with criminal pasts, unchecked by the state, is profoundly disturbing.
A Pattern of National Concern: The OIG’s Broader Scrutiny
The Colorado audit is not an isolated incident but rather part of a broader, ongoing series of seven Inspector General audits specifically examining state Medicaid payments for autism therapy across the nation. Four of these audits have been completed, with three remaining in progress. This systematic approach by the HHS OIG underscores a national concern about the potential for fraud, waste, and abuse in this specific area of Medicaid spending.

Previous audits in this series have already revealed substantial issues:
- Indiana: Estimated millions in improper and potentially improper payments.
- Wisconsin: Similar findings of significant financial irregularities.
- Maine: Also cited for substantial improper payments and oversight deficiencies.
Cumulatively, these previous audits estimated more than $120 million in improper payments and nearly $200 million in potential improper payments across Indiana, Wisconsin, and Maine. However, the potential fraud, waste, and abuse identified in Colorado’s Medicaid autism therapy payments proved to be the highest among all the completed audits to date, signaling a particularly acute problem within the state’s program.
The HHS OIG, as an independent oversight agency, plays a vital role in protecting the integrity of HHS programs and the well-being of beneficiaries. Its mandate includes detecting and preventing waste, fraud, and abuse; promoting economy, efficiency, and effectiveness; and informing the public and Congress about program performance and deficiencies. This series of audits demonstrates the OIG’s commitment to ensuring accountability in the multi-billion-dollar Medicaid program, a joint federal-state initiative that provides health coverage to millions of low-income Americans, including children with special needs.
Recommendations and Colorado’s Contested Response
In light of its findings, the Office of Inspector General issued several key recommendations to the state of Colorado:
- Refund of Federal Share: The OIG recommended that Colorado refund $42.6 million to the federal government, representing the federal portion of the identified improper payments. Medicaid is funded jointly by federal and state governments, with the federal share typically being around 50-70% depending on the state and specific services.
- Regular Facility Reviews: Implement regular, systematic reviews of autism facilities to ensure ongoing compliance with program rules and proper service delivery.
- Improved Guidance and Training: Provide better training and clearer guidance to therapy facilities on appropriate documentation practices and correct billing procedures for autism therapy.
Colorado’s response to the OIG’s recommendations was mixed. The state agreed to improve its guidance to providers and committed to conducting more regular reviews in the future, acknowledging the need for enhanced oversight and clarity. This indicates a recognition of the systemic issues identified by the audit.
However, Colorado vehemently disagreed with the recommendation to refund the $42.6 million. The state presented several arguments for its refusal:
- Limited Sample Size: Colorado contended that the audit’s findings were derived from a limited sample of claims, arguing that this sample was not sufficiently representative to extrapolate the total amount of improper payments across the entire program.
- Insufficient Detail on Errors: The state also argued that the audit lacked sufficient detail regarding the nature of specific errors, which they claimed made it difficult to fully understand and address the issues or to agree with the refund calculation.
- Lack of State Certification Requirement: Crucially, Colorado argued that its Medicaid program does not currently require the certification of behavior technicians before making payments. Therefore, they asserted that the refund calculation based on a perceived failure to ensure credentialed staff should be rescinded, as the state was not violating its own established regulations. This point highlights a significant disconnect between what might be considered best practice or federal expectation and existing state-level requirements.
This disagreement sets the stage for potential further discussions and negotiations between the federal OIG and the state of Colorado, or even a federal clawback of funds if the OIG maintains its position.
Broader Implications and Future Outlook
The findings of this audit carry profound implications, extending beyond the immediate financial figures and administrative disputes:
- Impact on Taxpayers: The estimated $285.2 million in improper and potentially improper payments represents a significant waste of taxpayer dollars, both federal and state. These funds are intended to provide essential healthcare services, and their misdirection erodes public trust in government programs.
- Integrity of the Medicaid Program: Such widespread irregularities undermine the integrity and credibility of the entire Medicaid program. If a program designed to serve vulnerable populations is plagued by such extensive waste and potential fraud, it raises questions about accountability across all aspects of its operation.
- Consequences for Beneficiaries: While the audit primarily focused on financial and administrative errors, the underlying issues directly impact the children receiving ABA therapy. Funds diverted through improper billing could have been used to expand access to care, improve the quality of services, or support other critical health initiatives. Moreover, the presence of unqualified or even dangerous staff directly jeopardizes the well-being and developmental progress of children with autism.
- Policy and Regulatory Reform: The audit serves as a powerful call for comprehensive policy and regulatory reform within Colorado’s Medicaid program for autism therapy. This includes strengthening oversight mechanisms, clarifying billing guidelines, implementing mandatory background checks for all staff interacting with vulnerable populations, and potentially reevaluating the state’s stance on credentialing requirements for behavior technicians.
- National Precedent: As part of a national OIG initiative, the Colorado audit’s findings will likely influence other states to review their own Medicaid autism therapy programs. It underscores the ongoing challenge of balancing broad access to care with robust program integrity in complex healthcare systems. The increasing prevalence of autism diagnoses and the rising demand for ABA therapy necessitate careful stewardship of resources to ensure that the services are effective, ethical, and sustainable.
The path forward for Colorado will involve navigating the immediate financial demands from the federal government while undertaking a significant overhaul of its oversight and administrative practices. The agreement to improve guidance and conduct more regular reviews is a positive step, but the refusal to refund monies based on existing state regulations highlights a deeper systemic issue that may require legislative action or a re-evaluation of state standards to align with best practices for patient safety and program integrity. The ultimate goal must be to ensure that every dollar spent on autism therapy in Colorado Medicaid genuinely contributes to the well-being and development of the children it is intended to serve, in an environment that is both safe and accountable.



